Cardiovascular Disorders
CLICK ON A TOPIC BELOW TO LEARN MORE
Aortic Stenosis
Aortic stenosis is a narrowing of the aorta (the large artery that distributes blood from the heart). The condition is congenital (present at birth) and is most common in German Shepherds, Boxers and Newfoundlands. Signs may include fatigue, cough, stunted growth, fainting and/or sudden death. Diagnosis is afforded through physical exam, electrocardiography, echocardiography and chest x-rays. Treatment includes medical management for heart failure although many cases can be corrected with open heart surgery. This surgery requires a heart-lung bypass, is relatively risky and quite expensive.
Arterial Thromboembolism
Arterial thromboembolism is a disorder of the heart and blood whereby blood clots (thrombi) form within the heart and then travel through the bloodstream until they become lodged. Commonly the thrombi lodge where the aorta divides toward the rear of the body (especially in cats). Causes of the emboli are degenerative arterial disease (eg. atherosclerosis), anatomical disorders (eg. vascular torsion), heart disease (eg. hypertrophic cardiomyopathy), bacterial infections, clotting disorders, kidney disease (glomerular loss of antithrombin III), metabolic disease (eg. Cushing’s disease), inflammation of arterial walls (arteritis), heartworm disease, trauma and chemical injury (eg. chemotherapy, drugs). Signs include abdominal pain, cold limbs (eg. hindlimbs of cats), lameness, ataxia, trouble breathing, coughing, seizure, coma and/or death. Diagnosis is afforded by physical exam, imaging studies (including doppler ultrasound), complete blood count, blood chemistries, special laboratory tests, heartworm tests and coagulation panels. Treatment may include clot busters (tissue plasminogen activator, streptokinase) if used within the first 12 hours of thrombus development devoid of hemorrhage. Other treatment may include surgery, anti-inflammatories and correction of associated disorders.
Autoimmune Hemolytic Anemia
The immune system affords the pet defense against foreign items such as infectious agents, injured cells and products of disease. It regulates antibody production and other defense components. In autoimmune hemolytic anemia, this defense system attacks normal red blood cells, causing severe life threatening anemia. Causes of the disease include metabolic disorders, neoplasia, infection, inflammatory disease, trauma and/or toxins. Signs include weakness, dyspnea (trouble breathing), anorexia, listlessness, depression, sensitivity to cold, vomiting, diarrhea and/or icterus (yellow mucous membranes). Diagnosis is afforded via complete blood count, blood chemistries, immune tests, urinalysis, direct Coomb’s test and physical exam. Treatment may include removal of the inciting agent, immunosuppressive drugs, anti-cancer drugs, surgery (splenectomy), plasmapheresis (removal of plasma and antibodies, then retransfusion of the red blood cells) and blood transfusion (only as a last resort due to inciting more blood destruction).
Autoimmune Thrombocytopenia
The immune system affords the pet defense against foreign items such as infectious agents, injured cells and products of disease. It regulates antibody production and other defense components. In autoimmune thrombocytopenia, this defense system attacks normal thrombocytes (cell components that help plug bleeding sites). This results in multiple hemorrhage. Signs include bleeding from various body sites. Diagnosis is afforded by physical exam, complete blood count, blood chemistries, urinalysis, clotting panels, bone marrow cytology and specific immune tests (eg. platelet factor-3 test, bone marrow direct fluorescent antibody (DFA) test). Treatment may include glucocorticoids plus danazol (reduces platelet destruction), vincristine (increases platelet release), blood and plasma transfusion, splenectomy (reduce platelet destruction and removal) and vincristine-loaded platelet transfusion.
Cardiac Arrhythmias
Cardiac arrhythmias are abnormalities in the rate or rhythm of the heart beat. There are many types of arrhythmias. Causes include degenerative disorders, congenital (present at birth) abnormalities, metabolic disorders, neoplasia, infectious disorders, inflammatory diseases, trauma and toxins. Their consequences range from mild to life threatening. Diagnosis is afforded by electrocardiography (ECG), auscultation, physical exam and echocardiography. Treatment includes medical management, surgery and/or pacemaker placement.
Congestive Heart Failure
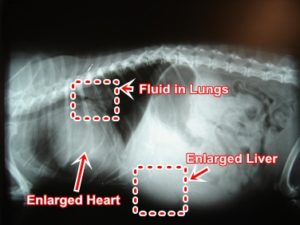
Congestive heart failure occurs when the heart does not pump enough blood to meet normal needs. Causes include heart valve disease, heartworm disease and/or congenital (present at birth) heart defects. Signs include coughing, shortness of breath, listlessness, abdominal fluid (ascites), cyanosis (bluish color of tongue), collapsing and/or death. Diagnosis is afforded by physical exam, auscultation, electrocardiography (ECG), echocardiography, chest x-rays and laboratory tests. Treatment is directed at removing accumulated fluids, diminishing the heart’s workload and increasing the heart’s efficiency. Drugs used include diuretics, ACE inhibitors and inotrophic agents.
Dilative Cardiomyopathy
Dilative cardiomyopathy is where weakened heart muscle causes the heart to enlarge (dilate) and pump inefficiently. This disease is seen more in large breed dogs over 3 years of age. Causes of the disease are unknown but may be associated with inflammatory disease, toxins, lack of essential cellular nutrients (eg. taurine in cats) and/or congenital defects. Signs include coughing, shortness of breath, listlessness, abdominal fluid (ascites), cyanosis (bluish color of tongue), collapsing and/or death. Diagnosis is afforded by physical exam, auscultation, electrocardiography (ECG), echocardiography, chest x-rays and laboratory tests. Treatment is directed at removing accumulated fluids, diminishing the heart’s workload and increasing the heart’s efficiency. Drugs used include diuretics, ACE inhibitors, anti-arrhythmic drugs and inotrophic agents.
Endocarditis
Endocarditis is inflammation of the lining of the heart walls and/or valves. Causes of the disorder is usually due to an infection from another part of the body. Infectious agents gain access and/or originate from periodontal disease, tonsils, kidneys, septic arthritis, bone infections, external wounds, gastrointestinal and/or respiratory infections. The most common sites affected are the mitral and aortic valves. Signs include murmur, fever, lethargy, depression, anorexia, shaking “chills” and/or death. Diagnosis is afforded via physical exam, complete blood counts, blood chemistries, autoimmunity tests, blood cultures, urinalysis and cardiac studies (eg. echocardiography). Treatment may include antibiotics, dental work, anti-inflammatories and heart medication.
Heartworm Disease
Heartworm disease is a parasitic disease of the lung arteries and heart. The disease is caused by the parasite Dirofilaria immitis which is transmitted to dogs and cats (as well as any warm blooded mammal) from infected dogs via mosquito.
Life cycle: Female mosquitos acquire first stage larvae (microfilariae) from infected dogs. Larvae develop within the mosquito to third stage larvae in approximately two weeks. Third stage larvae infect the dog or cat via mosquito bite. Larvae migrate and develop into fifth stage larvae (young adults) over approximately the next three months. Young adult Dirofilaria immitis worms enter the small pulmonary (lung) arteries 5-6 months postinfection. Through an immune-mediated, host inflammatory reaction, pulmonary arteries are damaged followed by worm infestation and damage of the host’s heart.
Signs of heartworm disease include exercise intolerance, coughing, trouble breathing (dyspnea), hemoptysis (spitting up blood), fainting and/or sudden death. Diagnosis is afforded via physical exam, blood filter tests, antibody tests, chest x-rays, complete blood counts, blood chemistries and imaging studies. Treatment is best directed toward prevention prior to infection (after a negative screening for the disease). If heartworm disease is detected, treatment includes an adulticide (eg. melarsomine dihydrochloride), anti-inflammatories and hospital support. The key is annual testing and monthly preventative treatment.
Hypertrophic Cardiomyopathy
Hypertrophic cardiomyopathy is an abnormal thickening (hypertrophy) of the heart muscle. This thickening diminishes the heart’s ability to pump adequate amounts of blood by limiting filling, impairing proper contraction and producing arrhythmias. The disease may strike males or females of any age, but is most common in middle aged male cats. Causes include viral infection, immune mediated reactions, toxins, nutrient deficiency and hyperthyroidism. Signs include listlessness, shortness of breath, fluid accumulation in the lungs, cough, anorexia, blood clots (see thromboembolism) and sudden death. Diagnosis is afforded via physical exam, complete blood count, blood chemistries, thyroid tests, echocardiography and chest x-rays. Treatment is directed at correcting any underlying disorders, removing accumulated fluid and improving the function of the heart.
Patent Ductus Arteriosus
The lungs of the developing fetus are not functional. Instead, the fetus receives oxygenated blood from its mother through placental circulation. Blood bypasses the fetal lungs via a blood vessel (the ductus arteriosus) and flows directly to the rest of the body. A small amount of blood flows through the fetal lungs. Normally at birth, the lungs inflate, the ductus closes and the offspring’s blood flows through the lungs acquiring oxygen for the rest of the body. In some pets, the bypass does not close at birth (patent ductus arteriosus), blood continues to bypass the lungs and not acquire oxygen. These pets are affected by insufficient oxygen. This birth defect occurs more in Shetland Sheepdogs, Poodles, Collies and Pomeranians than other breeds. Cats can also be affected. Signs may be subtle and unnoticed by the owner. Others include cough, stunted growth, exercise intolerance, collapse, death due to congested heart failure. Treatment includes correcting secondary problems (eg. lung congestion) and surgical closure of the ductus. Corrected early by experienced surgeons, the procedure is very successful and the long term prognosis is excellent.
Pericarditis/Pericardial Effusion
The pericardium is a thin sac that surrounds the heart and contains only a very small amount of fluid. Pericarditis is an inflammation of the pericardium. Pericardial effusion is a large accumulation of fluid within the pericardial sac. This effusion compresses the heart and inhibits its pumping ability. Pericardial effusion often develops because of pericarditis. Causes of pericarditis include heart failure, diaphragmatic hernia, abnormal blood clotting, neoplasia, inflammatory diseases, infections (bacterial, viral,fungal), trauma and toxins. Signs may include anorexia, vomiting, diarrhea, weight loss, abdominal pain, cough, dyspnea (trouble breathing), wheezing, listlessness and death. Diagnosis is afforded via physical exam, chest x-rays, imaging studies (eg. ultrasound), fine needle aspiration and cytology, electrocardiography, laboratory tests, complete blood count and blood chemistries. Treatment includes drawing excess fluid out of the pericardial sac (percardiocentesis) and surgery (eg. pericardectomy).
Persistent Right Aortic Arch (vascular ring anomaly)
During fetal development, certain large blood vessels disappear prior to birth. When parts of these vessels remain after birth, they can entrap the esophagus (food tube) and/or trachea (windpipe). This can interfere with passage of food and/or air. Signs of these disorders may include vomiting, regurgitation, weakness, dyspnea (trouble breathing), coughing and weight loss despite a good appetite. Diagnosis is afforded via accurate history, physical exam, chest x-rays and endoscopy. Treatment is best accomplished by surgery and secondary medical management.
Pulmonic Stenosis
Pulmonic stenosis is a congenital (present at birth) narrowing of the pulmonary artery that impairs blood flow from the right side of the heart to the lungs. This results in less blood reaching the lungs for oxygenation and the heart having to pump harder against the resistance. Signs of this disorder intensify with age whereby young puppies may show no signs but by 3 years of age, untreated pets exhibit full blown heart failure. Signs may include dyspnea (trouble breathing), listlessness, exercise intolerance, fainting, coughing, fluid accumulation (eg. abdomen, limbs) and death. Diagnosis is afforded by accurate history, physical exam, complete blood count, blood chemistries, doppler ultrasonography/echocardiography and chest x-ray. Treatment is directed at managing secondary disorders (eg. fluid accumulation, heart dysfunction). Surgical correction is an option (eg. patch graft, surgical or balloon valvuloplasty, pulmonary valvulectomy).
Valvular Insufficiency
Heart valves normally allow blood to flow in only one direction (through the heart). If a valve does not close completely (valvular insufficiency), blood flows back into the chamber from which it originated. This diminishes forward flow and produces back pressure at the overloaded area (eg. heart chamber, lungs, venous system). The disorder may affect the right, left or both sides of the heart. Signs of left sided heart failure include dyspnea (breathing trouble), coughing and exercise intolerance. Signs of right sided heart failure include decreased appetite, weight loss, abdominal fluid (ascites), vomiting, diarrhea and swollen limbs. Diagnosis is afforded by physical exam, auscultation, echocardiography (including doppler), chest x-rays, electrocardiography, complete blood count and blood chemistries. Treatment may include the elimination of accumulated fluid (eg. furosemide), ACE inhibitors, oxygen, vasodilators, inotrophic drugs and special diet.